- LOGIN
- MemberShip
- 2026-05-01 09:22:43
- Company
- Global pharmas showcase results at ARVO 2025
- by Cha, Jihyun May 08, 2025 06:08am
- The Association for Research in Vision and Ophthalmology (ARVO 2025) began on May 4 (local time) in Salt Lake City, Utah, USA. ARVO is the world's largest meeting of vision and ophthalmology researchers, attracting over 10,000 participants each year, and ARVO 2025 is being held over five days at the Salt Palace Convention Center. The exhibition hall was packed with attendees on the second day, May 5, when the main oral presentations and symposia took place. The slogan for this year's meeting is 'i3: Imagining Innovation and Intelligence in Vision Science,' and sessions focusing on convergent technologies such as artificial intelligence (AI), gene therapy, and regenerative medicine have been greatly expanded. ARVO 2025 More than 200 companies and institutions, including global big pharmas, are exhibiting this year. AbbVie (USA), Boehringer Ingelheim (Germany), Genentech (USA), and Regeneron (USA) each opened booths to showcase their latest technologies and ophthalmic pipelines. ZEISS (Germany) and Astellas (Japan) also promoted high-resolution retinal imaging systems, ocular drug delivery platforms, and patient-customized diagnostic solutions. ARVO 2025 Regeneron, a biotech with a leading global position in ophthalmic diseases, set up its promotional booth at the very center of the exhibition. At ARVO 2025, Regeneron emphasized 'Eylea (aflibercept),' its high-dose formulation for macular degeneration. Eylea HD is a new, high-volume product launched by Regeneron ahead of the original Eylea patent expiry, extending the dosing interval from every eight weeks to every 16 weeks. Regeneron is presenting 27 abstracts at ARVO 2025, eight oral presentations. In particular, Regeneron highlighted Eylea HD's market competitiveness by reporting the results of a meta-analysis, indirectly comparing it with Roche's competitor 'Vabysmo (faricimab).' ARVO 2025 Alcon displayed surgical and vision-care products for various ophthalmic conditions, including cataracts, glaucoma, retinal diseases, and refractive errors. Precision Vision drew attention by allowing attendees to try its virtual reality (VR)–based vision testing tools firsthand. Precision Vision has over 60 years of history in vision testing and visual function assessment equipment. LUXA Biotechnology, a subsidiary of Korea's Y2 Solution, drew particular interest by presenting clinical results for its dry age-related macular degeneration (AMD) therapy. LUXA was established in 2019 through Y2 Solution's investment and a joint venture with the U.S.'s first independent stem cell research institute, NSCI. Y2 Solution currently holds a 50% stake. At this meeting, LUXA presented preclinical data for its dry AMD cell therapy candidate 'RPESC-RPE-4W.' RPESC-RPE-4W is an adult retinal pigment epithelial stem cell (RPESC)–based therapy in which mature RPE cells derived from RPESCs are transplanted into the patient's subretinal space to restore damaged vision. It is currently in Phase 1/2a clinical trials. ARVO 2025 The RPESC-RPE-4W preclinical session drew over 200 attendees, creating an electrifying atmosphere. The session room was packed even before the presentation began, and many attendees who could not find seats stood throughout the talk. Dr. Brigitte Arduini, who presented the preclinical data, said, "In animal models receiving subretinal transplants, RPESC-RPE-4W demonstrated stable cell engraftment without serious adverse reactions or tumor formation," and added, "The transplanted cells positively influenced photoreceptor preservation and retinal structure maintenance, showing potential for functional vision improvement." Dr. Arduini added, "RPESC-RPE-4W showed minimal immune rejection post-transplant, suggesting high immunocompatibility consistent with adult-derived cell characteristics. These preclinical results will provide critical evidence for future clinical studies and open up new possibilities for treating dry AMD."
- Company
- Supreme Court rules in favor of Pharmbio’s Elpag Tab
- by Nho, Byung Chul May 07, 2025 06:02am
- On the 30th, Pharmbio Korea announced that it had won the final appeal in the patent dispute with Novartis, the patent holder of the original drug Revolade (eltrombopag olamine), for its immune thrombocytopenia treatment Elpag (eltrombopag olamine). Pharmbio Korea filed a request for a judgment on the scope of rights for 3 formulation patents in July 2023 and secured two consecutive victories in April 2024 (Intellectual Property Trial and Appeal Board) and December 2024 (Patent Court). The Supreme Court's ruling also upheld Pharmbio Korea's final victory. Pharmbio Korea has already obtained marketing authorization for the orphan drug Elpag and released it on October 1, 2024, with a reimbursement price of KRW 22,849 for Elpag 25 mg, KRW 22,849 for Elpag 25mg, and KRW 44,405 for Elpag 50mg, which is 30% lower than the price of the original product, significantly reducing the medical expenses for patients. Elpag is the first generic drug developed for the treatment of immune thrombocytopenia and severe aplastic anemia in Korea, achieving the localization of a product that Korea had previously relied on imported medications. Bong-kil Nam, CEO of Pharmbio Korea, stated, “A homegrown treatment for immune thrombocytopenia was urgently needed for patients with rare diseases. By localizing this medication, Pharmbio Korea has been able to reduce patients' costs by 30%.”
- Company
- Roche seeks reimb for Polivy as first-line DLBLC therapy
- by Eo, Yun-Ho May 07, 2025 06:02am
- Polivy, a first-line treatment for DLBCL introduced in 20 years, is seeking reimbursement listing in Korea. According to industry sources, Roche Korea recently submitted an application for reimbursement for Polivy (polatuzumab vedotin), a treatment for recurrent or refractory diffuse large B-cell lymphoma (DLBCL). Polivy originally sought reimbursement listing in 2021 for its first indication, as third-line treatment in combination with BR therapy (bendamustine and rituximab), but failed to pass the Health Insurance Review and Assessment Service's Cancer Disease Deliberation Committee review. Then in the first half of 2023, the company submitted an application for reimbursement for its use as first-line treatment in combination with the so-called R-CHP therapy, which includes rituximab+cyclophosphamide, doxorubicin, and prednisone, but was again rejected by the CDDC in February last year. Therefore, it remains to be seen whether Polivy, which has failed reimbursement listing twice in Korea, will be successful in gaining reimbursement this time. There is some optimism. The company added results from a 60.9-month follow-up analysis of the POLARIX study, which evaluated the efficacy of the Pola-R-CHP combination therapy in first-line treatment for DLBCL. The study, which was presented at the American Society of Hematology (ASH) 2024 Annual Meeting, was the first clinical trial in 20 years to expand the first-line standard of care for DLBCL. Key results showed that patients treated with the Polivy combination therapy demonstrated a significant improvement in overall survival (OS) compared to the control group treated with the standard R-CHOP. The lymphoma-related mortality rate was 9.0% in the Polivy combination therapy group and 11.4% in the R-CHOP control group. At approximately 5 years after treatment initiation, the risk of death in the Polivy combination therapy group was reduced by 15%, an improvement over the previous 3-year follow-up results (6% reduction in risk). Also, the Polivy combination therapy group (38.7%) required subsequent treatment (radiation therapy, systemic chemotherapy, CAR-T cell therapy, etc.) at a rate approximately 25% lower than the R-CHOP control group (61.7%). Diffuse large B-cell lymphoma is an aggressive form of blood cancer and the most common type of non-Hodgkin lymphoma. In South Korea, it is estimated that approximately 5,000 new patients are diagnosed with diffuse large B-cell lymphoma each year. Diffuse large B-cell lymphoma, which accounts for the highest proportion of non-Hodgkin lymphoma, is an aggressive type of lymphoma that requires immediate treatment due to its rapid progression. While over half of patients achieve remission with good treatment response rates, 30–40% do not respond to standard therapy (R-CHOP) or experience recurrence after initial treatment. Despite the fact that most patients experience relapse within 2 years and have a survival period of only 6 months upon relapse, relapsed or refractory diffuse large B-cell lymphoma remains an area with limited effective treatment options.
- Company
- Reimb for Pfizer Korea’s Lorviqua extended to first-line
- by Whang, byung-woo May 07, 2025 06:02am
- Pic of Lorviqua Pfizer Korea announced that Lorviqua (lorlatinib) will be reimbursed by health insurance for the first-line treatment of anaplastic lymphoma kinase (ALK)-positive metastatic non-small cell lung cancer (NSCLC) starting May 1. Lorviqua is a third-generation ALK tyrosine kinase inhibitor (TKI) designed to be effective against ALK mutations that were designed to easily cross the blood-brain barrier (BBB). In May 2022, it was granted reimbursement as a first-line treatment, 3 years after the indication was expanded to include ALK-positive metastatic non-small cell lung cancer as a first-line treatment. Patients with ALK-positive non-small cell lung cancer account for over 80% of all lung cancer cases and are characterized by relatively young age and a history of minimal or no smoking. Professor Sang Wee Kim, Professor of Oncology at Asan Medical Center, said, “It is important to treat ALK-positive metastatic non-small cell lung cancer with effective drugs based on accumulated clinical results from the early stages due to its characteristics. The reimbursement of Lorviqua is welcome news for patients who have not been able to receive proper treatment due to reimbursement restrictions, and there are high expectations in the medical field.” According to the 5-year follow-up results of the global Phase III CROWN clinical trial, Lorviqua demonstrated an 81% reduction in the risk of disease progression or death compared to the crizotinib group in patients with no prior treatment experience. Additionally, the median progression-free survival (PFS) for Lorviqua was not reached at 60.2 months of follow-up, regardless of brain metastasis status, while the median PFS for crizotinib was 9.1 months at 55.1 months of follow-up. According to an analysis of the CROWN 5-year results, this is the longest progression-free survival rate achieved among ALK-positive non-small cell lung cancer treatments to date. The safety profile of Lorviqua was consistent with the primary analysis, and no new safety signals were identified at the 5-year mark. Efficacy and safety were also consistently maintained in studies involving Asian patients. “Due to the nature of ALK-positive metastatic non-small cell lung cancer, there is a high unmet need among patients whose quality of life may be reduced due to brain metastases. It is meaningful that the reimbursement of Lorviqua as a first-line treatment will improve access to treatment for patients in Korea,” said Jin-Jeong Oh, Marketing Lead of the Oncology Business Unit at Pfizer Korea. Oh added, “Pfizer Korea will continue to strive to create significant changes in patients' lives and improve the treatment environment through various innovative therapies.”
- Company
- Reimb extension of anticancer drug combos imminent
- by Moon, sung-ho May 02, 2025 05:56am
- With the government announcing a major overhaul of its reimbursement policy for the use of anticancer drug combination therapies, there are various predictions on what specific methodology would be adopted. Curiosity is also growing about the scope of reimbursement that will be granted among the numerous combination therapies available, as well as when it will be applied. #In particular, as the MOHW has only announced the overhaul without providing any specific details, pharmaceutical companies, healthcare professionals, and patients are paying close attention and offering various predictions. According to industry sources on the 28th, the Ministry of Health and Welfare recently announced a partial amendment to the “Detailed Standards for the Application of Medical Care Benefits” with the main focus on improving the reimbursement policy for combination therapies. If confirmed as is, the amendment will be applied starting next month. The key point of the amendment is to completely change the reimbursement method for combination therapies, which has recently emerged as a major option in cancer treatment. Over the past five years, a total of 54 combination therapies using anticancer drugs have been approved in Korea. Among these, 28 involved adding new drugs to existing ones, while 26 involved combining two new drugs. However, if a new drug that is not covered by insurance is added to a drug that is already covered, it is considered a new therapy, and the existing drug is also no longer covered, placing a significant burden on patients. Furthermore, as combination therapy has become a trend in new drug development not only in Korea but also in the global market, controversy has repeatedly arisen whenever a new combination is approved in Korea. Amidst this controversy, the MOHW decided to add the following content to the revised notice: “In cases where anticancer therapy already granted reimbursement is used in combination with other anticancer drugs, the existing coinsurance rate shall apply to the existing anticancer therapy.” The MOHW added, ”In accordance with the HIRA announcement that the drug administration standards for anticancer therapy will be changed, the cost burden regulations will also be revised accordingly.” For reference, the MOHW also provided HIRA's contact information instead of its own in the administrative notice. Following the administrative notice, patient groups and related organizations such as the KRPIA unanimously welcomed the MOHW's policy. However, as no further details have been provided, questions surrounding the specific methodology are growing. Based on the announcement alone, it is unclear whether all anticancer drugs that are currently reimbursed regardless of indication will immediately be granted the same coverage when used in combination with other anticancer drugs starting in May. Even if individual treatments are currently covered by reimbursement, if they are approved for new indications when used in combination and are not covered by reimbursement, there is uncertainty as to which of the treatments will be covered by reimbursement after the administrative notice is finalized. This naturally leads to the question of whether the more expensive or less expensive one of the two drugs will be reimbursed. In addition, there are questions about whether combination therapies that have been approved by the MFDS based only on progression-free survival (PFS) data without overall survival (OS) data will be reimbursed under the MOHW's new policy. Accordingly, the industry, especially the multinational pharmaceutical companies, is paying close attention to the HIRA Cancer Disease Deliberation Committee meeting scheduled for the 30th. If the MOHW administrative notice is finalized at the end of this month, the industry expects the additional details to be announced at the CDDC meeting held at the end of April. At a CDDC meeting in October last year, HIRA established deliberation principles for discussing whether to approve reimbursement for major combination therapies and has been gathering opinions from relevant academic societies. A CDDC member, who is a university hospital professor, said, “In previous discussions, HIRA did not allow the use of drug A with reimbursement and drug B with 100% coinsurance just because their combined use was approved by the MFDS. Instead, we decided to discuss it if a request was made through the collection of opinions from academic societies.” He added, ”Even if it is approved by the MFDS if reimbursement is granted as is, it will cause problems with insurance finances, so this would require the Cancer Drug Review Committee’s control.” He added, “We were originally scheduled to discuss the opinions on combination therapy reimbursement proposed by each academic society at the end of this month. We will focus on the recommendations made in the guidelines for anticancer drugs, but it is questionable whether it is possible to switch all the recommended therapies to reimbursement at once given the current situation.” This is why there are concerns in the frontline about what will happen if the MOHW's announcement is implemented in May. Some are fearing possible reimbursement cuts. With the MOHW's policy on combination therapy announced, a series of inquiries have already been pouring in from patients during outpatient visits. A professor of hematology and oncology at a tertiary hospital, who requested anonymity, said, “HIRA has gathered opinions on the reimbursement of combination therapy through academic societies, but it is still questionable whether everything can be applied in May. I am concerned that there will be cuts when we file the claims.” He added, ”In the case of multiple myeloma, combination therapy is always used for each stage of treatment. Moreover, the number of high-priced treatments has been increasing recently,” he said, expressing his concern, ”If reimbursement cuts are made, hospitals will suffer considerable damage. We must prepare for all possibilities.” As a result, if the MOHW's policy is applied as is to clinical practice, the sequencing itself, including the number of treatment sequences, will differ for each type of cancer. A pharmaceutical industry official explained, “Although this policy is being promoted specifically for anticancer drugs, issues of equity with other diseases are bound to arise in the future. If this policy is limited to anticancer drugs, the entire sequencing in clinical practice will change. If some drugs are used in the first line because they are reimbursed, there may be cancer types for which there are no treatment options that can be used with reimbursement in the second line.” The insider concluded, “Considering all these factors if the May notice is finalized, it could cause significant confusion in practice and the pharmaceutical industry. While patients may welcome this development, it is an issue that requires more systematic discussion.”
- Company
- Will Ebglyss benefit from the reimb changes in Korea
- by Eo, Yun-Ho May 02, 2025 05:56am
- With the tide turning in favor of allowing switching between atopic dermatitis treatments in Korea, all eyes are on whether Ebglyss will be able to emerge as a new player in the market. According to industry sources, Eli Lilly Korea accepted a price less than the evaluated amount(lower than the weighted average price of substitute drugs) set for Ebglyss (lebrikizumab) presented by the Drug Reimbursement Evaluation Committee of the Health Insurance Review and Assessment Service in February and is currently negotiating drug prices with the National Health Insurance Service. If Ebglyss is listed, there will be 6 treatment options available for atopic dermatitis in Korea. The options include the biological agents (injectables) “Dupixent (dupilumab)” and “Adtralza (tralokinumab),” and JAK inhibitors (oral) “Rinvoq (upadacitinib),” “Civinqo (abrocitinib),” and “Olumiant (baricitinib).” The health authorities have recently been considering whether to allow JAK inhibitors to be used in cases where patients do not respond adequately to existing treatments (biological agents) or have poor tolerability, which is expected to further intensify market competition. If approved, Ebglyss will immediately benefit from the regulatory changes. It was approved by the Ministry of Food and Drug Safety in August 2024 for the treatment of moderate-to-severe atopic dermatitis in adults and adolescents 12 years of age and older (weighing at least 40 kilograms) who are inadequately controlled by topical treatments or for whom such treatments are not recommended. Ebglyss demonstrated its clinical efficacy and safety profile in a pivotal Phase III clinical trial. Patients who achieve a clinical response after 16 weeks of treatment can thereafter receive a maintenance dose (250 mg) every 4 weeks, making it a useful first-line treatment option for patients with atopic dermatitis in Korea. The clinical studies on which the license was based are the Phase III ADvocate-1, ADvocate-2, and ADhere trials. The trials evaluated the clinical efficacy and safety of Ebglyss in 1062 adults and adolescents with moderate-to-severe atopic dermatitis. In ADvocate-1 and ADvocate-2, which evaluated Ebglyss as a monotherapy, Ebglyss improved outcomes, with 58.8% and 52.1% (16.2% and 18.1%, respectively in the placebo arm) achieving Eczema Area and Severity Index (EASI) 75; and 38.3% and 30.7% (9% and 9.5%, respectively in the placebo arm) achieving EASI 90 during the induction period (weeks 0-16) compared to placebo. Also, after one year of maintenance therapy (Week 52), 81.7% of the Ebglyss arm achieved EASI 75 (vs. 66.4% in the placebo arm) and 66.4% achieved EASI 90 (vs. 41.9% in the placebo arm), demonstrating significant symptom improvement in the long term.
- Company
- New dementia drug Leqembi expands prescriptions in KOR
- by Eo, Yun-Ho May 02, 2025 05:55am
- Despite being a non-reimbursed drug, the Alzheimer's treatment Leqembi is being actively prescribed in Korea. According to industry sources, Eisai Korea's Leqembi (lecanemab) is now available for prescription at major tertiary hospitals including Samsung Medica Center, Seoul National University Hospital, Asan Medical Center, and Sinchon Severance Hospital, as well as other medical institutions such as Gachon University Gil Hospital, Korea University Guro Hospital, Busan Paik Hospital, and Ilsan Gospel Hospital. Since its official launch late last year, the drug has been rapidly expanding its prescription scope in Korea. Leqembi has been proven to reduce the rate of disease progression and slow cognitive decline by selectively binding to amyloid beta (Aβ) aggregates, which are a known cause of Alzheimer's disease. Due to the lack of treatments for the disease, the desperation of the patients and their families had been indescribable. In addition to public petitions, the MFDS's Korea Orphan & Essential Drug Center has been inundated with inquiries on the date of Leqembi’s approval and supply in Korea. However, the problem is the price of the drug. In the U.S., Leqembi costs about KRW 35 million per year; in Japan, it costs KRW 27 million. Due to its high price, it will take a while for the drug to be approved in Korea and be listed for reimbursement as it requires a tug-of-war between pharmaceutical companies and the government. In the Clarity AD study, Leqembi achieved statistically significant results in both its primary and secondary endpoints. Specifically, Leqembi delayed clinical decline in brain function by 27% at 18 months compared to placebo. While the market for amyloid-targeted therapies such as Leqembi is gaining recognition for its effect in delaying the onset of dementia, the use of the drug has been hampered by its characteristic side effects. The amyloid-related imaging abnormalities (ARIA) that are often mentioned as an issue, are abnormal signals observed on MRI scans, such as brain edema or microhemorrhage that are detected with the drug’s use. Depending on how the adverse event occurs, ARIA is classified as ARIA-E and ARIA-H. ARIA-E can be observed on MRI as brain edema or sulcal effusions, and ARIA-H as microhemorrhage and superficial siderosis. Meanwhile, Leqembi has recently received approval from the European Commission (EC). As a result, Leqembi has become the first new Alzheimer's disease drug with a novel mechanism of action to be approved in Europe.
- Company
- Entry of oral GLP-1 obesity drug imminent...Novo vs Lilly
- by Son, Hyung Min Apr 30, 2025 06:11am
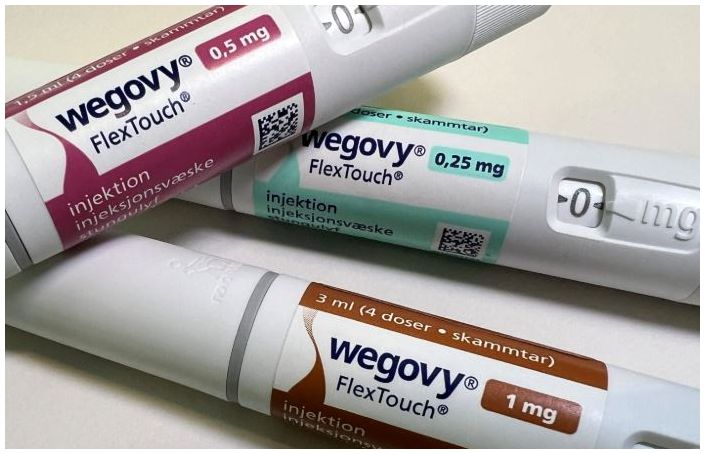
- The launch of an oral GLP-1 class obesity drug is imminent. Novo Nordisk recently completed a Phase III clinical trial for its oral obesity drug candidate and submitted a marketing authorization application to the U.S. Food and Drug Administration (FDA). Eli Lilly, a competitor of Novo Nordisk, is also developing an oral GLP-1 class drug candidate, orforglipron, as a successor to Zepbound. Lilly has confirmed significant weight loss effects of its candidate in a Phase III clinical trial. In addition, domestic and international pharmaceutical companies such as Viking Therapeutics, Ildong Pharmaceutical, and D&D Pharmatech are also actively developing oral GLP-1 drugs. Novo and Lilly complete Phase III trials side by side According to industry sources on the 28th, Novo Nordisk has completed a Phase III clinical trial for its oral semaglutide-based obesity drug candidate and recently submitted a marketing authorization application to the FDA. The pharmaceutical industry has been racing to develop new formulations since GLP-1 class obesity treatments such as Saxenda, Wegovy, and Zepbound emerged as global blockbuster drugs. The existing drug Saxenda requires once-daily administration, while Wegovy and Zepbound require weekly injections. Oral formulations are expected to gain a competitive edge in terms of convenience of administration. Novo Nordisk, which developed the oral diabetes drug Rybelsus containing semaglutide, has also begun developing an oral obesity drug. In the OASIS1 clinical trial, which confirmed the weight-loss effect of oral semaglutide, a 50mg dose of the compound demonstrated a 15% reduction in body weight compared to placebo over 68 weeks. This result was statistically significant compared to the placebo group, and adverse reactions were comparable to those observed in previous injectable clinical trials. Novo Nordisk is also developing a combination oral formulation of GLP-1 and amylin analog to stay ahead of the competition. According to clinical results disclosed to date, the average weight loss effect of this new drug candidate at week 12 was 12%. Eli Lilly has also recently disclosed the results of a Phase III clinical trial for its oral GLP-1 agent. Lilly's investigational drug, orforglipron, demonstrated simultaneous effects on HbA1c and weight loss. In the Phase III clinical trial named ACHIEVE-1, orforglipron 36 mg (once daily) reduced HbA1c by an average of 1.5% over 40 weeks. During the same period, the placebo group saw a reduction of only 0.1%. Additionally, the orforglipron group showed an average weight loss rate of 7.9%, compared to 1.6% in the placebo group, demonstrating a significant difference. In terms of safety, no significant adverse reactions were observed beyond the gastrointestinal side effects that are characteristic of GLP-1 class drug. The rate of treatment discontinuation due to adverse effects was 8% in the orforglipron 36 mg group, higher than the 1% in the placebo group, but most were mild-to-moderate in severity. No serious adverse reactions, such as liver toxicity, were reported. Lilly is preparing to submit a marketing authorization application for the obesity indication of orforglipron by the end of this year, with the diabetes indication targeted for submission in 2026. Lilly aims to shift the paradigm of the GLP-1 market, which has been dominated by injectable formulations, by leveraging orforglipron. Lilly expects a strong response from the medical field, as orforglipron is an oral small molecule drug with manufacturing ease and supply flexibility. In fact, Lilly has already invested billions of dollars in expanding its production infrastructure in the U.S. since last year to prepare for the global launch of orforglipron. Novo Nordisk and Lilly lead the oral obesity drug pathway, with Viking and Ildong among other domestic and international pharmaceutical companies in pursuit Semaglutide-based obesity drugsIn addition to Novo Nordisk and Lilly, Viking Therapeutics, Ildong Pharmaceutical, and D&D Pharmatech are also actively developing oral GLP-1 drugs. Viking Therapeutics recently announced the results of a Phase I clinical trial of VK2735, an oral candidate drug targeting GLP-1/ glucose-dependent insulinotropic polypeptide (GIP). This study evaluated the safety and tolerability of VK2735 in healthy adults with a body mass index (BMI) of 30 kg/m² or higher, who received a single daily dose of VK2735 for 28 days. The clinical results demonstrated encouraging safety and tolerability of VK2735 at a maximum daily dose of 40 mg. In detail, VK2735 at 40 mg showed a maximum weight loss effect of 5.3% compared to baseline. In terms of safety, all treatment-related adverse events reported in participants who received VK2735 were mild-or-moderate. The majority (76%) were mild, and vomiting, one of the representative side effects of obesity drugs, was not reported. Viking Therapeutics plans to confirm the potential of VK2735 through a Phase II clinical trial Yunovia, a new drug research and development subsidiary of the Ildong Pharmaceutical, is conducting a Phase I clinical trial on ID110521156, a new drug candidate in the GLP-1 receptor agonist class targeting metabolic diseases such as diabetes and obesity. ID110521156 is a small molecule drug, and the company aims to develop it as an oral synthetic new drug for diabetes and obesity with distinct advantages over existing representative treatments, such as peptide injections, including superior productivity and excellent ease of use. Previously, Yunovia confirmed the efficacy of its candidate’s insulin secretion and blood sugar control through preclinical efficacy and toxicity evaluations. Its candidate also demonstrated superior safety compared to competing drugs in the same class and confirmed promising drug characteristics in the recently completed Phase I single-ascending dose (SAD) trial. D&D Pharmatech is collaborating with U.S.-based Metsera on the development of an oral obesity drug. Previously, Metsera entered into a technology transfer agreement with D&D Pharmatech in April 2023 to acquire the rights to 'DD02S,' an oral GLP-1-based peptide obesity treatment candidate, and 'DD03,' an oral GLP-1, GIP, and glucagon receptor triple agonist obesity treatment candiate. The first patient dosing for a Phase I/II clinical trial on DD02S was completed in North America last November. D&D Pharmatech confirmed that DD02S demonstrated more than 12.5 times higher absorption rate than the currently marketed oral GLP-1-based obesity treatment ‘Rybelsus (semaglutide)’ in preclinical studies.
- Company
- K-pharma unveils results on TPD to ADC at AACR
- by Son, Hyung Min Apr 30, 2025 06:07am
- The Korean pharmaceutical and biotech industry has shown achievements in developing anticancer drugs equipped with novel mechanisms. They demonstrated potential in areas that have rapidly risen as R&D trends, such as targeted protein degraders, antibody-drug conjugates (ADCs), and bispecific antibodies. According to industry sources on the 29th, the American Association for Cancer Research Annual Meeting (AACR 2025) began on the 25th and will run for five days in Chicago, USA. The AACR is classified as one of the world’s top three oncology conferences, along with the American Society of Clinical Oncology (ASCO) and the European Society for Medical Oncology (ESMO). The annual meeting primarily features early‐stage clinical results for anticancer drug candidates, such as preclinical and phase 1 data. Dong-A ST·Therapex demonstrated achievements in preclinical trials involving TPD Companies such as Dong-A ST, Therapex, Pin Therapeutics, and Nibec unveiled their development results for targeted protein degraders (TPDs) at this meeting. While conventional small‐molecule therapies inhibit protein function, TPD drugs are designed to fundamentally degrade and remove disease-causing proteins, offering superior therapeutic efficacy and eliminating resistance issues. TPD drugs's advantage lies in their ability to target over 80 % of disease-causing proteins that cannot be modulated by conventional small‐molecule compounds. Dong-A ST unveiled preclinical results for its EGFR-targeted protein degrader 'SC2073' at this meeting. Currently available EGFR-positive lung cancer treatments include first-generation Iressa (gefitinib, AstraZeneca) and Tarceva (erlotinib, Roche), second-generation Giotrif (afatinib, Boehringer Ingelheim) and Vizimpro (dacomitinib, Pfizer), and third-generation Leclaza (lazertinib, Yuhan) and Tagrisso (osimertinib, AstraZeneca). However, resistance often develops even with highly effective targeted therapies. The C797S mutation is a key resistance mechanism in EGFR-positive treatment. Moreover, treatment options remain limited after resistance to targeted therapies emerges. For patients with resistance to targeted therapies, options such as platinum-based chemotherapy, docetaxel, or immuno-oncology agents are available, but response rates show no significant improvement. SC2073 acts on an allosteric binding site of EGFR and selectively degrades only the mutant EGFR forms that are resistant to existing non-small cell lung cancer (NSCLC) therapies. It does not affect normal EGFR, thereby minimizing associated side effects. Therapex unveiled data on its degrader antibody–drug conjugate (DAC) 'TRX-214-1002,' which links a GSPT1 molecular glue to a CD33 antibody, at AACR 2025. DACs are expected to offer higher safety than ADCs because they employ TPDs, small molecules that degrade proteins. ADCs are novel anticancer drugs that connect an antibody, which binds to specific antigens on the surface of cancer cells, with a cytotoxic drug linked by a linker. ADCs use antibodies' selectivity for their targets and the drug's cytotoxic activity to selectively target cancer cells, thereby increasing therapeutic efficacy while minimizing side effects. While Roche's Kadcyla, the first-generation ADC, is only approved for breast cancer, second-generation ADCs are approved for various indications. Enhertu and Trodelvy have been shown to be effective in various solid cancer areas, such as breast cancer, non-small cell lung cancer (NSCLC), and colorectal cancer. Despite its high intracellular target specificity and ability to induce decreased protein expression, TPD has low in vivo utilization. Developers are conducting clinical trials to use TPD and ADC for precise target identification. AACR 2025 Therapex is developing TRX-214-1002 as a treatment for acute myeloid leukemia (AML) that is refractory to existing therapies or has low drug responsiveness. In July of last year, it received support from the Korea Drug Development Fund (KDDF) to advance its development. TRX-214-1002 attaches a GSPT1 payload to the same antibody used in the ADC therapeutic 'Mylotarg.' Preclinical results showed that TRX-214-1002 demonstrated improved outcomes in AML treatment compared with conventional ADC therapies. Pin Therapeutics has unveiled the preclinical research results for 'PIN-5018' for the first time. PIN-5018 is a molecular glue degrader targeting CK1α (Casein Kinase 1 alpha), operating via a mechanism that blocks cancer cell survival pathways. Pin Therapeutics has unveiled the preclinical research results for 'PIN-5018' for the first time. PIN-5018 is a molecular glue degrader targeting CK1α (Casein Kinase 1 alpha), operating via a mechanism that blocks cancer cell survival pathways. CK1α is a serine/threonine kinase that plays essential roles in cell cycle regulation, DNA repair, immune responses, and other vital functions. PIN-5018 works by suppressing cancer cell growth and survival through induction of the degradation of this protein. PIN-5018 is being developed specifically for MSS (Microsatellite Stable) colorectal cancer, which has a low response rate to immuno-oncology drugs. MSS-type colorectal cancer accounts for approximately 80–85% of all colorectal cancers. Still, it is classified as an area of high unmet need because current response rates to immuno-oncology drugs or targeted therapies are low, and the duration of response is short. Pin Therapeutics reported that PIN-5018 demonstrated superior antitumor efficacy compared to existing first-line therapies in preclinical studies and showed positive potential as a monotherapy and in combination regimens. Yuhan·Celltrion·Aptamer Sciences presented preclinical results for ADCs and bispecific antibodies Yuhan and ABL Bio presented preclinical data on 'YH32364' (ABL104) in a poster session at this AACR meeting. YH32364 is designed as a bispecific antibody that simultaneously targets EGFR and 4-1BB. EGFR is a well-known biomarker expressed in major solid tumors, including non–small cell lung cancer (NSCLC) and colorectal cancer. By simultaneously targeting EGFR and T-cell activating 4-1BB, Yuhan aims to maximize the antitumor effect of this immuno-oncology candidate. Yuhan reported that in a preclinical efficacy trial, YH32364 showed stronger superior effects in EGFR-expressing tumors compared to cetuximab. It was demonstrated that the candidate drug retained long-term anti-tumor effects through immunological memory. Furthermore, it was confirmed that YH32364 activated 4-1BB signaling in EGFR-expressing tumors, leading to the recruitment of tumor-infiltrating immune cells and altering the tumor microenvironment. Cetuximab is an anticancer agent that targets the EGFR receptor and is used to treat various cancers, including colorectal cancer, head and neck cancer, and lung cancer. It is particularly well known to be effective in colorectal cancer patients with KRAS gene mutations. Yuhan stated that YH32364 works by activating immune cells through EGFR-specific 4-1BB signaling in tumors. The company hopes YH32364 will be more effective in a wide variety of EGFR-expressing solid cancers than anti-EGFR mAb. AACR 2025 Celltrion presented preclinical results for its multi-specific antibody-based anticancer drug candidate, 'CT-P72.' CT-P72 is a multi-specific antibody immunotherapy co-developed by Celltrion and Abpro, a biotechnology company based in the United States. This therapy is designed as a T-cell engager (TCE), which connects cancer cells that express HER2 (Human Epidermal Growth Factor Receptor 2) with T cells, a type of immune cell, to help eliminate the cancer cells. T-cell engagers are a bispecific antibody-based modality that physically links cancer cells and immune cells to treat cancer. This mechanism can harness the human immune system to attack cancer, enabling more precise targeting of cancer cells and eliciting a potent immune response. CT-P72 is designed to simultaneously target HER2 and the immune cell surface protein CD3 to activate T cells and attack cancer cells while minimizing toxicity to normal cells. In particular, it demonstrated high tumor inhibition by selectively acting on cancer cells in HER2-overexpressing tumor models. Moreover, CT-P72 consistently maintained its antitumor efficacy in both in vitro and in vivo studies, and in primate toxicity tests, it exhibited 180-fold superior safety compared to a reference compound. Aptamer Sciences presented pre-clinical results of its new ADC candidate product, 'AST-203.' AST-203 targets the protein TROP2, which is predominantly expressed in breast, pancreatic, gastric, and lung cancers. This drug candidate binds selectively to TROP2-positive tumors, penetrates the cells, and releases the microtubule inhibitor MMAE to induce cancer cell death. AST-203 is made by conjugating TROP2-targeting antibody with 'MMAE,' a microtubule disruption agent, with linker 'VC-PAB.' TROP2 is an intracellular calcium signal transducer involved in cell proliferation and survival. Among TROP2-targeting drugs, the commercialized products are Gilead's ADC Trodelvy and Daiichi Sankyo/AstraZeneca's Datroway. Both products are approved for breast cancer indications only. Because TROP2 is mainly found in breast cancer, NSCLC, colorectal cancer, and pancreatic cancer, later entrants are conducting clinical trials targeting these major solid tumors. Aptamer Sciences is exploring ways to overcome the limitations of existing ADC therapies using its proprietary ADC platform technology, 'Aptamer.' Aptamers are one-tenth the size of antibodies, allowing deeper penetration into tumor tissue and rapid delivery to target cells for therapeutic effect. In preclinical studies, Aptamer Sciences confirmed the potential of AST-203 in tumor spheroid models (three-dimensional aggregates of cultured cells). According to the company, AST-203 demonstrated a 6.7-fold higher tumor penetration rate than Trodelvy.
- Company
- ‘Policy support required for hidradenitis suppurativa’
- by Whang, byung-woo Apr 30, 2025 06:06am
- “Hidradenitis suppurativa is difficult to cure and requires long-term treatment. As it is a rare disease, I think it is desirable to increase access to treatments with clear treatment benefits by providing both reimbursement and special calculation for this disease, which has a small number of patients.” Hidradenitis suppurativa is a disease whose exact cause or pathogenesis has not yet been fully identified, and it is a rare disease with a prevalence rate of less than 1% in South Korea. The number of patients with hidradenitis suppurativa in South Korea is estimated to be approximately 10,000 as of 2022, which only includes those who have been clearly diagnosed after experiencing recurrent lesions and formation of tracts beneath the skin. Although TNF-α inhibitors are a reimbursable treatment option, options are limited when considering treatment failure and side effects. Joo Yeon Ko, Department of Dermatology, Hanyang University Medical CenterAt an interview with Dailypharm, Joo Yeon Ko, Professor of Dermatology at Hanyang University Medical Center emphasized the need to improve access by expanding treatment options for hidradenitis suppurativa. Hidradenitis suppurativa causes abscesses to form in various areas around the sebaceous glands beneath the skin. Unlike typical abscesses, the lesions are connected to each other, forming channels known as “tracts.” It is broadly classified into ▲active, where inflammation persists, and ▲inactive, where no further inflammation occurs; however, it is difficult to clearly distinguish between the active and inactive states. Professor Ko explained, “Even in the same patient, the condition can be highly active at one time and stable at another, so the medication and treatment methods used may vary depending on the individual's condition. In the case of active disease, the patient experiences severe pain due to inflammation in areas such as the armpits, and the goal of treatment is to reduce the frequency of the inflammation.” He continued, “Mild-to-moderate patients rarely visit university hospitals, and mild patients with symptoms in one or two areas are mainly treated at private clinics. It is important to identify the potential for progression to severe disease in mild patients, as a higher recurrence rate is associated with a higher risk of progression.” Limited treatment options for suppurative hidradenitis, IL-17 emerges but faces hurdles for use The basic treatment for suppurative hidradenitis is I&D (incision and drainage), which involves incising the area where the patient feels pain to remove the internal inflammation. In addition, antibiotics are administered for about 3 months to reduce inflammation, and if there is a high risk of recurrence, sebum inhibitors used to treat acne are also used. However, in severe cases, these treatments are not sufficient to control the inflammation, and biological agents are used. Currently, Humira (adalimumab), a TNF-α inhibitor, is covered by insurance. In addition, although not yet covered by insurance, the interleukin-17 (IL-17) inhibitor Cosentyx (secukinumab) was approved in Korea in 2015, approximately 8 years after the approval of Humira. Professor Ko said, “TNF-α inhibitors covered by insurance have the advantage of broadly blocking inflammation, but they also have the limitation of blocking the inflammatory response that is necessary for our bodies. IL-17 inhibitors have a more targeted mechanism than TNF-α inhibitors and show similar therapeutic effects and superior safety.” According to overseas and domestic guidelines, both TNF-α inhibitors and IL-17 inhibitors are currently recommended as first-line treatment options. If sufficient therapeutic effects are not achieved with oral medications, one of the two approved biological agents can be selected. Regarding this, Professor Ko explained, “Although TNF-α inhibitors have been covered by insurance in Korea for over 5 years, not many patients actually use them on-site. TNF-α inhibitors have a broad anti-inflammatory mechanism, which raises concerns about side effects, and when we explain this to patients, they are reluctant to use them.” In actual treatment, patients who received IL-17 inhibitors (Cosentyx) showed a significant improvement in quality of life after continuing treatment for one and a half years, said Professor Ko. Previously, patients had severe symptoms requiring surgery and were unable to move their arms properly, but after treatment, their symptoms improved significantly, and the use of antibiotics and other medications decreased to 25% of the previous level. Professor Ko stated, “In global clinical trials, approximately 60% of patients achieved HiSCR 50 with Cosentyx. This means that 60% of patients experienced a 50% or greater improvement in symptoms. While a 50% improvement may seem modest, it actually represents a significant improvement.” He added, “Hidradenitis suppurativa is a disease that develops at a young age and requires long-term management, so controlling it with medications that have few side effects is the best approach. In this regard, I believe Cosentyx is a good option at this point.” “Hidradenitis suppurativa, a rare and intractable disease pustular psoriasis…unrestricted special reimbursement calculation support is needed” However, there are restrictions on the use of the IL-17 inhibitor Cosentyx. Unlike Humira, which is covered by reimbursement, Cosentyx is not yet covered. In fact, Novartis Korea applied for reimbursement expansion for Cosentyx for hidradenitis suppurativa in November last year, but the discussions are at a standstill. Professor Ko said, “IL-17 inhibitors have already been used extensively in psoriasis, so there is a tendency to prefer Cosentyx, but it is difficult to use it actively because it is not covered by insurance. Currently, if TNF-α inhibitors are used and sufficient effects are not seen, the cost of using Cosentyx thereafter is extremely high.” Professor Ko emphasized that while it may be worth considering distinguishing treatment sequence within biological agents based on practical factors like drug prices, from a medical perspective, it is important to prioritize options that have fewer side effects. He said, “If TNF-α inhibitors are used in the first line and are not effective, using Cosentyx as a the next treatment option can be an alternative, but this cannot be considered the ideal approach from a medical standpoint. In the long term, it would be desirable to apply reimbursement so that both treatments can be used on an equal footing.” Additionally, Professor Ko stressed the need for policy support to apply special reimbursement calculation provisions for the rare and intractable disease suppurative hidradenitis. Currently, suppurative hidradenitis is classified according to severity, and only severe cases are eligible for special reimbursement and insurance coverage, but the total number of patients is only about 10,000, and among them, less than 1,000 are estimated to be severe cases. Therefore, even if reimbursement and special calculations are applied simultaneously, it is unlikely to place a significant financial burden on the government. Professor Ko said, “For diseases like hidradenitis suppurativa, which have a small number of patients and treatments offer clear benefits, it is necessary to increase access to treatment by providing both reimbursement and special calculations. Even if reimbursement and special calculations are applied simultaneously, only a few dozen patients will actually benefit and use Cosentyx each year.” Finally, he added, “Effective medications for treating hidradenitis suppurativa are continuing to emerge, and better ones will be developed in the future. I hope patients do not lose hope and actively consult with medical professionals and seek treatment.”