- LOGIN
- MemberShip
- 2026-04-29 01:43:10
- Company
- GSK’s myelofibrosis drug Omjjara faces reimb hurdles
- by Eo, Yun-Ho Oct 14, 2025 06:41am
- The reimbursment of GSK’s new myelofibrosis drug Omjjara has become uncertain in Korea. According to Dailypharm coverage, the reimbursement application for GSK Korea's myelofibrosis treatment Omjjara (momelotinib), which had passed the Cancer Disease Deliberation Committee of the Health Insurance Review and Assessment Service (HIRA) in March, was not placed on the agenda of the Drug Reimbursement Evaluation Committee. It appears that differences arose between GSK and HIRA over the selection of a comparator drug used for pricing, effectively halting Omjjara’s first reimbursement attempt. As a result, it remains to be seen whether GSK will resubmit a reimbursement application and proceed with the listing process. Omjjara has a triple mechanism of action that inhibits JAK1 and JAK2 as well as ACVR1 (activin A receptor type 1). In myelofibrosis treatment, JAK1 and JAK2 inhibition helps relieve systemic symptoms and reduce splenomegaly, while ACVR1 inhibition decreases hepcidin expression and thereby alleviates anemia. Anemia management remains one of the major unmet needs in treating myelofibrosis. Transfusion-dependent anemia brings more than just the commonly perceived issue of dizziness - depending on its severity, it can be life-threatening. Phase III trials SIMPLIFY-1 and MOMENTUM demonstrated that Omjjara significantly improved key symptoms such as splenomegaly and reduced transfusion dependence in anemic myelofibrosis patients regardless of prior JAK-inhibitor exposure. In SIMPLIFY-1, which compared Omjjara to ruxolitinib (Jakavi) in JAK-inhibitor-naïve myelofibrosis patients, Omjjara demonstrated non-inferiority to ruxolitinib in the primary endpoint of spleen volume response at week 24. The proportion of transfusion-independent patients was 66.5 % in the Omjjara group versus 49.3 % in the ruxolitinib group, showing a statistically significant reduction in transfusion dependence in the Omjjara arm. Professor Seo-yeon Ahn of Chonnam National University Hwasun Hospital’s Department of Hematology stated, “Existing JAK inhibitors relieve splenomegaly and systemic symptoms but often worsen anemia or increase transfusion needs, leaving an unmet clinical need. Omjjara demonstrated significant clinical value in improving anemia, which is closely tied to prognosis in myelofibrosis patients.”
- Company
- Hugel appoints Carrie Strom as global CEO
- by Chon, Seung-Hyun Oct 14, 2025 06:41am
- Hugel announced on October 13 that it has appointed Carrie Strom, a medical aesthetics leader and a former Senior Vice President at AbbVie, as its new Global CEO. Carrie Strom, HugelCarrie Strom will lead Hugel's global business operations. She is highly regarded as an expert in the aesthetics field, having served for five years, from May 2020 to February this year, as the Senior Vice President at the global pharmaceutical company AbbVie and the President of Allergan Aesthetics Global. Strom initially joined Allergan (now AbbVie) in 2011 and has since led the aesthetics portfolio, which includes the botulinum toxin product 'Botox' and the HA filler 'Juvéderm,' across more than 50 countries. Previously, she served as Senior Vice President of Allergan's U.S. Medical Aesthetics division and spent 11 years as a sales and marketing expert at Pfizer. Following the recent appointment of Jang Doo-hyun as the Chief Executive Officer for the Korean operations, Hugel plans to accelerate its growth, particularly in the Americas, with the addition of the new Global CEO. Carrie Strom stated, "I am excited to work with Hugel's talented and dedicated employees and Board of Directors," and added, "My top priority will be to build upon Hugel's leadership in Korea to become a global leader in the aesthetics market, raising the standards of service we provide to customers and patients worldwide." Suk-yong Cha, Chairman of Hugel's Board of Directors, stated, "CEO Carrie Strom is an expert who has gained extensive experience and driven change in the global medical aesthetics industry. We expect her to maximize Hugel's future value during this critical transition to a global enterprise, particularly in the Americas."
- Company
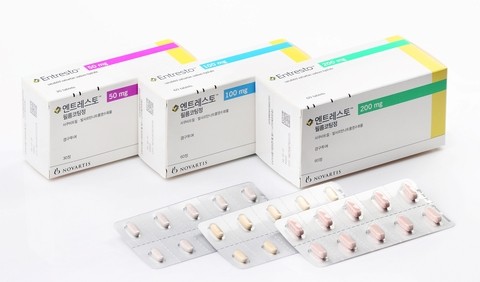
- Entresto patent dispute near its end, yet 0 generic approval
- by Kim, Jin-Gu Oct 14, 2025 06:40am
- Product photo of EntrestoThe patent dispute of Novartis' heart failure treatment, 'Entresto,' is nearing its final judgment. Still, generic companies may be unable to launch their products early, regardless of the ruling. To launch a generic early, companies need not only to win the patent dispute but also to secure product approval from the Ministry of Food and Drug Safety (MFDS). The MFDS is reportedly demanding supplementary data from the relevant generic companies. In other words, generic manufacturers, after fighting patent battles for five years, risk winning the legal fight only to be unable to launch their product. Not a simple combination drug but a 'cocrystal complex'...may be delaying generic approval According to the MFDS on October 13, there are currently zero product approvals for Entresto generics. This is considered unusual given that generic product approvals are typically processed within a year and a half of application. Approximately 10 generic companies involved in the Entresto patent dispute applied for generic product approval sequentially from April 2022 to July of the following year. They filed these applications based on their first-instance victory in the patent dispute. However, there has been no news of Entresto's generic product approval for almost 3 years. It is reported that the MFDS is requesting supplementary approval documentation. The pharmaceutical industry is paying attention to the MFDS's request for supplementation regarding Entresto's unique crystal structure. Entresto is a heart failure treatment in which the active ingredients, sacubitril and valsartan, act on cardiac neurohormones through separate pathways. The unique feature is that the two ingredients form a single crystalline structure, a cocrystal complex. Medicines combining two or more ingredients typically involve a simple mixture of the crystalline forms of each component. In contrast, a cocrystal involves two or more components bound together at the molecular level like a single compound. They exhibit single-compound properties until just before absorption into the body. For this reason, the industry refers to Entresto not merely as a 'combination drug' but as a 'complex' with a singular characteristic. The problem is the scarcity of approved generics for this cocrystal formulation. Entresto is reportedly the only drug approved as an API-API cocrystal complex, not only in Korea but also in the U.S. and Europe. Furthermore, there is no precedent anywhere in the world for the approval of a generic for a cocrystal complex drug. The MFDS is contemplating this issue. The Ministry is struggling to find an appropriate analytical method for generic approval. Critics suggest that because the cocrystal structure differs from traditional combination products in its physicochemical properties, applying the same analytical methods may not be suitable for generic approval. A pharmaceutical industry official said, "If it were a typical combination product's crystal form, there would have been no issue with approval, but I understand the MFDS is deeply concerned about whether it is appropriate to use existing methods to analyze this special cocrystal structure and grant generic approval." Winning in the Supreme Court, yet generic companies may face a failed launch Given the circumstances, companies preparing Entresto generics are now in a position where they may be unable to launch their products even if they win the final patent dispute. Generic companies initiated a declaratory judgment action against Novartis's Entresto crystal form patent in January 2021. This was followed by the filing of invalidation and circumvention trials against the use patent, salt/hydrate patent, and formulation patent. Generic companies won successive victories in the first and second instances. Disagreeing with these rulings, Novartis appealed the cases to the Supreme Court. Of the two cases appealed to the Supreme Court, the ruling in the use patent case was finalized in April of last year, with Novartis losing. The remaining pending case is the dispute over the crystal form patent. The full merits review is currently underway, following the dismissal without deliberation deadline in April of this year. Separately, the salt/hydrate patent dispute is awaiting a ruling from the Patent Court. The pharmaceutical industry reportedly anticipates that the final ruling regarding the crystal form patent could be issued as early as this year. If the Supreme Court sides with the generic companies, as in the first and second instances, the generic companies' patent risk would be effectively eliminated. However, regardless of the Supreme Court's decision, if MFDS approval continues to be delayed, generic companies will face a dual burden: winning a five-year-long dispute only to be unable to launch the product.
- Company
- Only Ozempic undergoes DREC review for reimb, not Mounjaro
- by Eo, Yun-Ho Oct 13, 2025 06:03am
- The reimbursement journey for the two diabetes drugs that have recently gained attention as obesity treatments is taking different paths, drawing industry interest. On October 2, the Health Insurance Review and Assessment Service (HIRA)’s Drug Reimbursement Evaluation Committee reviewed Novo Nordisk Korea’s Ozempic (semaglutide) but did not review Eli Lilly Korea’s Mounjaro (tirzepatide)—which had been widely expected to be reviewed simultaneously. Ozempic received a positive evaluation for reimbursement adequacy and passed the committee. The product had already accepted the “setting a price below the assessed value” condition when it first submitted the application in 2023, but the company had withdrawn the application due to supply issues during price negotiations with the National Health Insurance Service. Given that, many predicted its second review would pass smoothly under the same terms. The interesting part is the non-review of Mounjaro. Typically, when multiple drugs of similar classes apply for reimbursement listing for the same indication, the government conducts reimbursement evaluations for the drugs simultaneously to gain leverage in negotiations. This raises questions about the background and implications of this outcome. Since receiving domestic approval in 2023, Lilly has been under negotiations with the Health Insurance Review and Assessment Service (HIRA) for Mounjaro for a considerable period since early 2024. Throughout this process, Lilly has demonstrated confidence that it can prove the cost-effectiveness of Mounjaro by conducting a pharmacoeconomic evaluation based on the efficacy confirmed in the type 2 diabetes field, which was not conducted for Ozempic. Normally, new drugs establish cost-effectiveness through PE analysis and then negotiate prices based on the results. However, in markets like diabetes, where existing drugs have a solid presence and market entry speed is critical, pharmaceutical companies sometimes choose to accept the weighted average price of substitute drugs to hasten the process. But Lilly chose a different path. In the pivotal SURPASS clinical trial, which became the basis for approval, Mounjaro demonstrated statistically superior reductions in HbA1c and body weight compared to all control arms, including semaglutide (1 mg, brand name Ozempic), insulin degludec, and insulin glargine—showing potential for diabetes remission and underlining Lilly’s confidence. Furthermore, at the European Association for the Study of Diabetes (EASD) conference held last September, Lilly presented results from the SURPASS-CVOT Phase III clinical trial, which directly compared its GLP-1 receptor agonist Trulicity. This reinforced the data on cardiovascular prevention effects and overall survival improvement. Based on such circumstances, the Health Insurance Review and Assessment Service's (HIRA) decision to submit only Ozempic to the October Drug Reimbursement Evaluation Committee, rather than both drugs simultaneously, may not necessarily be a negative signal for Mounjaro. For Mounjaro, which has already undergone pharmacoeconomic evaluation, being assessed under different criteria than Ozempic could be advantageous. However, Mounjaro's future is not entirely bright. Korea’s reimbursement framework rarely applies a flexible ICER (Incremental Cost-Effectiveness Ratio) threshold for chronic disease indications, making it difficult for even innovative drugs to gain higher valuation. When Minister Eun Kyeong Jeong, who was appointed as the new Minister of Health and Welfare in the Lee Jae-myung administration last July, agreed to her National Assembly confirmation hearing on the need for policy changes to recognize the innovation of new drugs. She specifically mentioned Trodelvy as the first case of flexibly applying the ICER threshold. It remains to be seen whether the government's policy direction for innovative new drugs and the treatment of new drugs for chronic diseases, such as Mounjaro, will change. A Lilly representative stated, “Mounjaro offers differentiated clinical value compared to existing oral agents, insulins, and GLP-1 receptor agonists. We will continue to collaborate closely with health authorities and stakeholders to ensure that Mounjaro’s innovation can promptly benefit more Korean patients with diabetes.”
- Company
- Will gastric cancer-targeted therapy Vyloy pass CDDC review?
- by Eo, Yun-Ho Oct 10, 2025 06:06am
- Attention is focused on the second attempt for insurance reimbursement of the gastric cancer-targeted anticancer drug Vyloy. According to industry sources, Astellas Korea’s Vyloy (zolbetuximab), a Claudin 18.2-positive gastric cancer-targeted therapy, is currently coordinating its schedule for review by the Health Insurance Review and Assessment Service’s Cancer Disease Deliberation Committee. The application is expected to be listed on the agenda this month. Vyloy failed to pass CDDC review last February. Astellas resubmitted its reimbursement application in June. Approved in Korea in September last year, Vyloy is the first globally approved Claudin 18.2-targeted treatment, an immunoglobulin monoclonal antibody that binds to Claudin 18.2, a protein expressed and exposed in the stomach. According to the Phase III SPOTLIGHT study that became the basis of Vyloy’s approval, the median progression-free survival (mPFS) of the combination of Vyloy and mFOLFOX6 (oxaliplatin, leucovorin, fluorouracil) was 10.61 months, compared to 8.67 months for the placebo group. The median overall survival (mOS) was also longer—18.23 months versus 15.54 months in the placebo group. In the GLOW study as well, the combination of Vyloy and CAPOX (capecitabine plus oxaliplatin) achieved an mPFS of 8.21 months, reducing the risk of disease progression or death by approximately 31%. However, Vyloy remains non-reimbursed in Korea. It was listed for discussion at the CDDC in February, but failed to establish reimbursement standards. Additionally, a companion diagnostic issue delayed its launch in Korea until March this year. To use Vyloy, patients must be identified as Claudin 18.2-positive, but the companion diagnostic device (CDx) used for this test was under consideration for new medical technology evaluation. To address this, Astellas began an Early Access Program (EAP) even before approval so that patients in need could use the drug in advance. Currently, 51 patients across 10 institutions are enrolled. Professor Sun-Young Rha, Department of Medical Oncology at Yonsei Cancer Center, commented, “About 90% of metastatic gastric cancer patients are HER2-negative, and there has been a pressing need for new biomarker-targeted therapies. About 40% of HER2-negative patients are reported to be Claudin 18.2-positive, so the emergence of Vyloy, which selectively binds to Claudin 18.2, offers a new therapeutic possibility.”
- Company
- Boehringer wins 'Jardiance' generic trademark dispute
- by Kim, Jin-Gu Oct 10, 2025 06:05am
- Product photo of Jardiance In a trademark dispute over the generic-name trademark for the SGLT-2 inhibitor diabetes treatment, 'Jardiance (empagliflozin),' the original manufacturer has won a ruling from the Intellectual Property Trial and Appeal Board (hereafter, the Board). Analysis suggests that the Board's rare decision to rule in favor of the original company was based on the high similarity between the English brand name, 'Jardiance,' and the disputed generic trademark, 'Jadiance.' According to the pharmaceutical industry on the 4th, the Intellectual Property Trial and Appeal Board recently issued a ruling of 'acceptance' in the trademark nullification trial filed by Boehringer Ingelheim against Shinil Pharma. The trademark in question is 'Jadiance,' which Shinil Pharma filed in March 2022. Shinil Pharma applied for this trademark with a focus on generics for both Jardiance and Jardiance Duo. The trademark was registered in August 2023. Shinil Pharma subsequently received a priority marketing authorization for a Jardiance Duo generic under the name 'Jadiance Duo.' However, just two months after the 'Jadiance' trademark was registered, Boehringer Ingelheim filed a nullity action in October 2023. The Board sided with the original manufacturer after approximately two years of deliberation. With generics expected to launch simultaneously after the expiration of the Jardiance substance patent on the 23rd of this month, Shinil Pharma is now unable to launch its generic product under the name 'Jadiance Duo' due to the loss of the trademark dispute. Shinil Pharma must either receive a reversal ruling through an appeal to the Patent Court or secure a new product approval under a different trademark to launch its generic. In this regard, Shinil Pharma holds trademarks such as 'Januglia,' 'Janumetia,' 'Januxr,' and 'Empagl,' which are presumed to be for Jardiance and Jardiance Duo generics, and these are not subject to the current dispute. The ruling is being called exceptional, given the Board's precedents. While global pharmaceutical companies have brought numerous legal actions to protect the trademarks of their original drugs, the Board and the Supreme Court have generally been lenient toward generic companies. More recently, in May, Novartis lost a trademark nullification trial it filed against Elyson Pharmaceutical, arguing that the generic name 'Entrelto' was too similar to its heart failure treatment, 'Entresto.' Similarly, Boehringer Ingelheim filed nullification trials in 2020 against Kwangdong Pharmaceutical's 'Dijenta' and Daewoong Pharmaceutical's 'Traceta' for being too similar to its diabetes treatment, 'Trajenta,' but those trials were also dismissed. Even the trademark dispute between 'Gliatirin' and 'Gliatamin' was ultimately decided in favor of the generic company by the Supreme Court. Meanwhile, the original company won the latest dispute, which is unlike past rulings and decisions. In this regard, the pharmaceutical industry notes that the Board found a high degree of similarity between Jardiance's English brand name, 'Jardiance,' and Shinil Pharm's 'Jadiance.' The global product name is 'Jardiance.' Both the U.S. FDA and the European Medicines Agency (EMA) approved the original empagliflozin-containing diabetes treatment under the product name 'Jardiance.' However, when Boehringer Ingelheim introduced the product in Korea, the company obtained product approval under the Korean spelling of "Jardiang" rather than the English pronunciation 'Jardiance.' Despite this, the approved English product name remains 'Jardiance,' identical to the global name. The company's registration with the Ministry of Intellectual Property only includes the Korean name "Jardiang", not 'Jardiance.' In this context, it is also explained that Boehringer Ingelheim only filed a trademark nullification trial against Shinil Pharma's 'Jadiance.' It has been confirmed that Shinil Pharma's 'Jadiance' is the only case currently involved in a trademark dispute with Boehringer Ingelheim over Jardiance and Jardiance Duo.
- Company
- Boryung acquires global rights to Taxotere for KRW 288B
- by Chon, Seung-Hyun Oct 02, 2025 06:13am
- Boryung acquired global rights to Sanofi's anticancer drug ‘Taxotere’ for up to KRW 287.8 billion. This investment, approaching KRW 300 billion, secures a revenue stream of approximately KRW 100 billion in annual sales. Boryung announced on the 30th that it has signed a global licensing agreement with Sanofi for the global business of the cytotoxic anticancer drug ‘Taxotere’ (docetaxel), including domestic and international rights, distribution rights, licensing rights, production rights, and trademark rights. The deal is valued at up to EUR 175 million (KRW 287.8 billion). Of this, EUR 161 million (KRW 264.8 billion) will be paid at closing, while the remaining EUR 14 million (KRW 23 billion) will be contingent on achieving certain contractual milestones. Through this acquisition, Boryung will take over the comprehensive business operations of Taxotere in 19 countries, including Korea, China, Germany, and Spain, as well as in Latin America and the Middle East, subject to approval by local regulatory authorities. Once regulatory procedures are completed, Boryung plans to manufacture Taxotere at its Yesan Campus and directly distribute and market the drug in global markets. Docetaxel is listed on the WHO Model List of Essential Medicines, and Taxotere is the original brand product of docetaxel. First approved by the U.S. FDA in 1995, Taxotere has been widely used for the treatment of various solid tumors, including breast cancer, prostate cancer, gastric cancer, and head & neck cancers. According to Sanofi, the product generated global sales of EUR 70 million (KRW 115.4 billion) last year. Even today, the clinical utility of Taxotere continues to expand, particularly in combination therapies, reinforcing its role as a key component in global cancer treatment. A Boryung representative explained, “Although the paradigm in oncology is shifting toward targeted and immuno-oncology therapies, cytotoxic agents remain a fundamental backbone of cancer treatment.” Boryung has previously taken over the domestic operations of global original oncology drugs such as Gemzar (2021) and Alimta (2023), successfully transitioning them to in-house production and ensuring stable supply. Boryung aims to advance as a global pharmaceutical company in the field of cytotoxic anticancer drugs through the acquisition of the Taxotere business. A Boryung official emphasized, “In the actual global market, repeated stockouts and supply disruptions of cytotoxic anticancer drugs are impacting patient treatment. Through this acquisition of the Taxotere global business, we plan to expand our differentiated portfolio in the cytotoxic anticancer drug field by stably establishing the global supply chain for these essential medicines, whose importance has grown.” Jeong-Gyun Kim, CEO of Boryung, said, “Boryung has gone beyond simple product acquisitions, internalizing manufacturing and formulation improvements to secure sustainable competitiveness. The Taxotere global business acquisition marks not only our third anticancer drug takeover after Gemzar and Alimta, but also the first time we have acquired global rights to an original medicine, paving the way for full-scale overseas expansion.” Kim added, “We will advance Taxotere's therapeutic value by expanding beyond simple technology transfer into comprehensive R&D, including follow-up formulation development, combination therapy strategies, and research into new indications. Through this, we aim to strengthen our differentiated portfolio in the cytotoxic oncology field, directly manufacture and distribute original anticancer medicines on the global stage, and reinforce our future growth engines.”.
- Company
- Severe asthma drug 'Fasenra' enters 'Big 5' gen hospitals
- by Eo, Yun-Ho Oct 02, 2025 06:11am
- Product photo of Fasenra 'Fasenra,' a treatment for severe asthma, is now available by prescription at tertiary general hospitals. According to industry sources, AstraZeneca Korea's Fasenra (benralizumab) passed the drug committees (DC) of 'Big 5' general hospitals, including Samsung Medical Center (Seoul), Seoul National University Hospital, Seoul Asan Medical Center, Seoul St. Mary's Hospital, and Sinchon Severance Hospital. Fasenra was included in the insurance reimbursement list in July of last year. The drug can be reimbursed when treating patients with severe eosinophilic asthma who are inadequately controlled despite treatment with high-dose inhaled corticosteroid-long-acting beta-agonist (ICS/LABA) and long-acting muscarinic antagonist (LAMA). Specifically, the following criteria should be met: ▲Within the year before starting treatment, the eosinophil count in the blood was 300 cells/㎕ or higher, and within the first year of treatment, systemic oral corticosteroids (OCS) were required for acute exacerbations four or more times, or within 6 months before starting therapy, systemic oral corticosteroids were continuously administered, or ▲The eosinophil count in the blood was 400 cells/㎕ or higher within the year before starting treatment. Systemic corticosteroids were required for acute exacerbations three or more times within the first year of treatment. Severe eosinophilic asthma accounts for approximately 84% of severe asthma cases. It involves frequent exacerbations and may lead to reduced quality of life despite treatment with high-dose inhaled corticosteroids and other conventional therapies. In particular, when symptoms are not controlled, even with asthma controllers, oral steroids may be necessary. However, long-term use of these medications is associated with systemic side effects such as osteoporosis, hypertension, and diabetes. Therefore, biological agents are recommended to reduce the dosage of these treatments. Fasenra is a targeted biologic agent that binds directly to interleukin-5 receptor alpha (IL-5Rα) expressed on eosinophils' surface, inducing cell apoptosis. It has been demonstrated to reduce blood eosinophil counts rapidly within one day of administration. Meanwhile, in the results from the global Phase 3 SIROCCO clinical trial, enrolling 1,205 severe eosinophilic asthma patients worldwide, including those in Korea, Fasenra administered at 8-week intervals showed a 51% reduction in annual asthma exacerbation rates compared to placebo after 48 weeks of treatment. In the CALIMA study, Fasenra treatment also resulted in a 28% reduction in annual asthma exacerbation rates compared to placebo.
- Company
- CKD to exclusively sell Bayer’s heart failure drug Verquvo
- by Chon, Seung-Hyun Oct 02, 2025 06:11am
- Chong Kun Dang announced on the 1st that it has signed an exclusive sales agreement with Bayer Korea for the chronic heart failure treatment ‘Verquvo’. Under the agreement, Chong Kun Dang will handle the exclusive distribution, sales, and marketing of Verquvo at domestic hospitals and clinics starting this month. Verquvo is a treatment for symptomatic chronic heart failure in patients with a left ventricular ejection fraction (LVEF) of less than 45%. It is the world’s first soluble guanylate cyclase (sGC) stimulator approved for chronic heart failure. The drug directly stimulates the nitric oxide–sGC–cGMP pathway, demonstrating efficacy in improving vascular function and enhancing cardiac structure and function. In global clinical trials, Verquvo was shown to reduce the risk of cardiovascular death and hospitalization due to heart failure in high-risk chronic heart failure patients who had experienced worsening of symptoms despite standard therapy. It is evaluated as presenting a new treatment paradigm for high-risk patient groups, acting through a mechanism distinct from existing neurohormone blockade-centered therapies. Chong Kun Dang and Bayer Korea have been long-standing partners. Since 2005, they have co-promoted antibiotics such as Cifrobay and Avelox, and since last year, they have co-marketed Kerendia, a treatment for chronic kidney disease associated with type 2 diabetes. In February 2024, Chong Kun Dang also began exclusive sales of Bayer’s progressive hepatocellular carcinoma treatments Nexavar and Stivarga in Korea, further strengthening their partnership. Young-Joo Kim, President of Chong Kun Dang Pharma, said, “Chong Kun Dang has been leading the cardiovascular disease treatment market based on its extensive experience and expertise in the field. With the exclusive sales of Verquvo, we will be able to establish a differentiated portfolio in the field of chronic heart failure treatment and provide patients with broader therapeutic options.” JinA Lee, President/CEO of Bayer Korea, said, “Since Verquvo was reimbursed under the national health insurance in September 2023, it has become a cornerstone treatment for patients experiencing worsening heart failure symptoms. Through our collaboration with Chong Kun Dang, we hope more Korean patients with chronic heart failure can benefit from Verquvo’s proven clinical value.”
- Company
- Servier Korea appoints Olivier Russo as new General Manager
- by Son, Hyung Min Oct 02, 2025 06:11am
- Olivier Russo, new General Manage of Servier Korea Servier Korea announced that it has appointed Olivier Russo as its new General Manager, effective October 1. Olivier Russo, the new GM, is a pharmacist and R&D expert who earned his PhD in Organic Chemistry and Medicinal Chemistry from the Université Paris-Saclay in France. Since joining the Servier Group in 2006, he has demonstrated leadership across core R&D functions throughout the entire drug lifecycle—from early-stage discovery of novel drug candidates to technology development, industrialization, and post-approval stages. Since 2022, Russo has served as Global Head of CMC, where he led company-wide strategy and operations. He successfully supported the initiation of clinical trials and regulatory approvals for key pipeline candidates in oncology, neuroscience, and immunology/inflammatory diseases, as well as the full lifecycle management program for cardiovascular and metabolic disease treatments. The new GM said, “Korea not only holds a strong presence in key areas for Servier, such as cardiovascular and metabolic diseases, but is also emerging as a new leader in targeted cancer therapy. As part of Servier's Asia-Pacific R&D hub, Korea is also a strategic center for strengthening the clinical development foundation in the region.” He added, “We will strive to combine the strengths of the Korean market with Servier's global expertise to deliver greater value to patients worldwide, while driving sustained innovation.” Servier is an independent global pharmaceutical group managed by a non-profit foundation. Headquartered in France, it has a strong global presence in over 140 countries. Driven by its mission to advance treatments that meet patient needs, it focuses approximately 70% of its R&D budget on oncology, providing innovative medicines primarily in oncology and cardiovascular and metabolic diseases.