- LOGIN
- MemberShip
- 2026-04-30 17:45:16
- Policy
- Daewoong joins in competition in the Forxiga generic market
- by Lee, Tak-Sun Mar 26, 2024 06:30am
- Daewoong Pharmaceutical, which had been in charge of the domestic sales and marketing of the original SGLT-2 diabetes drug ‘Forxiga (propanediol hydrate),’ is belatedly entering the generic market through a transfer and acquisition deal. Daewoong had sold Forxiga until January this year. It is analyzed that Daewoong also entered the generic market after AstraZeneca announced its plan to withdraw the drug from the Korean market in the second half of this year. According to the industry on the 5th, Daewoong Pharmaceutical will be listing its Forxiga generic ‘Forxilo Tablet 5mg' at a ceiling price of KRW 262 from April through a transfer and acquisition. Daewoong reportedly acquired Zalozin Tab 5mg from NBK Pharm. The drug is produced by Dongkoo Bio&Pharma upon consignment. Daewoong also acquired the license for Forxilo 10mg in January through an assignment and transfer deal Daewoong did not enter the generic market when Forxiga’s patent expired in April last year because it was selling the original Forxiga Tab at the time. Daewoong has been in charge of domestic sales and marketing of AstraZeneca's Forxiga since March 2018. The company continued to sell Forxiga even after launching its SGLT-2 class drug Envlo (enavogliflozin) in May last year. However, its ties with AstraZeneca ended at the end of the past year with AstraZeneca’s announcement that it will discontinue sales of Forxiga in Korea. In January, Daewoong stopped the distribution and sales of Forxiga, and HK Inno.N took over. Daewoong's entry into the generic market is expected to change the competitive landscape of the market. In particular, generic companies are expected to compete fiercely for the remaining pie once the original withdraws from the domestic market in the second half of the year. Although Daewoong is focusing on promoting its own new drug Envlo, the pharmaceutical industry believes that the power and experience the company had accumulated selling the original Forxiga for 6 years is a force to be reckoned with. Another factor that will affect the market structure is that from April 8, the generic pricing premium applied to innovative Forxiga generic drugs will end. This is because the reduced drug price is likely to reduce promotion costs. However, the pricing premium will be maintained on April 8, 2026, for salt-modified drugs produced by three or fewer generic companies.
- Policy
- Pfizer tops global mkt…Samsung Biologics tops Korean mkt
- by Lee, Hye-Kyung Mar 26, 2024 06:30am
- In 2022, global pharmaceutical giant Pfizer and Korean pharmaceutical giant Samsung Biologics took the top spots in terms of sales, earning KRW 91 billion and KRW 2.437 trillion, respectively. in 2022, according to a new report released by the Korea Health Industry Development Institute, According to the '2023 Health Industry Statistics' recently published by the Korea Health Industry Promotion Institue, sales in the domestic pharmaceutical industry totaled at KRW 37.69 trillion in 2022, up 12.8% year-on-year from KRW 33.42 trillion in the previous year. On the other hand, R&D expenditures the companies invested company granted for each employee totaled at KRW 314.9 billion in the same year, up a mere 6.4% year-on-year. When looking at the sales of the 'Big 5' companies, Pfizer brought in over KRW 91 billion in global pharmaceutical sales and ranked first, followed by AbbVie's KRW 56 billion, then Johnson & Jones, Novartis, and Merck's earnings of KRW 50 billion each. Domestic pharmaceutical companies surpassed the 'KRW 1 trillion club' threshold, with Samsung Biologics posting sales of KRW 2.437 trillion, Celltrion Pharm KRW 1.937 trillion, Yuhan Corp KRW 1.7264 trillion, Chong Kun Dang KRW 1.4723 trillion, and GC Biopharma KRW 1.2449 trillion. In terms of the overall domestic pharmaceutical industry market size, in 2022, the global pharmaceutical industry was valued at USD 1.357 trillion and the domestic pharmaceutical industry was valued at USD 22 billion (KRW 28.905 trillion), showing a -7% difference compared to 2021. The slowdown in growth is expected to continue until 2023. According to the statistics compiled by KHIDI, the global pharmaceutical industry, which has been showing -3% growth ($139.2 billion in the global market and KRW 21 billion in the Korean market) by 2023, will recover its sales from this year and increase market size by 8.3% to reach USD 1.478 trillion and KRW 26 billion, respectively. The top 10 countries in the global pharmaceutical industry in 2022 were the United States with 30.7% (KRW 416 billion), China with 14.4% (USD 196 billion), and Japan with 6.9% ($93 billion), and KHIDI recorded 1.6% ($22 billion), ranking 12th in the world. In 2022, Korea exported $8.083 billion worth of drugs and imported $8.795 billion, with exports going to the U.S. grossing USD 986 million, Japan at USD 772 million, and Germany at USD 773.6 million. In terms of domestic imports, Germany accounted for the most at $1.578 billion, followed by the United States’ USD 1.154 billion and China’s KRW 957 million. Meanwhile, in 2022, a total of 619 domestic drug manufacturers produced a total of 28.953 trillion won (KRW 25.572 trillion from finished drugs and KRW 3.379 trillion in raw materials.) In the domestic pharmaceutical industry, 788.85 people, with 61.4% of them working at workplaces with 300 or more employees.
- Policy
- Sotyktu, Livtencity to be reimb from April
- by Lee, Jeong-Hwan Mar 25, 2024 05:59am
- Sotyktu for plaque psoriasis and Livtencity 200 mg for cytomegalovirus (CMV) infection will be newly listed for reimbursement from the 1st of next month. GLP-1 receptor agonists (GLP-1 RAs, single-agent therapy, and combination therapy) will be reimbursed for use in combination with basal insulin therapy when a patient’s HbA1c level is 7% or higher, even with the use of metformin combination therapy. Reimbursement for the macular degeneration drug Beovu will be extended to cover diabetic macular edema, Rinvoq to moderate-to-severe active ulcerative colitis in adults, Cellcept to connective tissue disease-associated interstitial lung disease, and Soliris to optic neuromyelitis optica spectral disorder (NMOSD). The Ministry of Health and Welfare (MOHW) announced a notice on the partial amendment to the details of the criteria and methods for the application of reimbursement benefits (pharmaceuticals) that contained the changes above on the 22nd. A new reimbursement standard will be set for BMS’s psoriasis drug Sotyktu. Patients with chronic severe plaque psoriasis are eligible. Takeda Pharmaceutical’s Livtencity will be reimbursed for the treatment of cytomegalovirus (CMV) infection and disease following solid organ transplantation or hematopoietic stem cell transplantation. GLP-1 receptor agonists (GLP-1 RAs, single-agent therapy, and combination therapy) will be reimbursed for use in combination with basal insulin therapy when a patient’s HbA1c level is 7% or higher, even with the use of metformin combination therapy. Macular degeneration treatment Beovu will be reimbursed based on the same standards set for anti-VEGF agents in diabetic macular edema (up to 14 total doses per patient, including ranibizumab, faricimab, and aflibercept). Rinvoq’s reimbursement will be extended to cover treatment for adults with moderate-to-severe active ulcerative colitis. For the use of interleukin inhibitors and TNF-α inhibitors criteria set for its use in plaque psoriasis, the previous treatment criteria for the use of MTX or cyclosporine has been expanded to include "DMF administered in patients who were expected to have adverse reactions to MTX or cyclosporine or who are unable to continue treatment due to adverse reactions. Cellcept will be reimbursed for connective tissue disease-related interstitial lung disease, in addition to systemic neuropathy. The serum level criteria that had been applied to fertility medications such as Pergoveris and Luveris will be removed.
- Policy
- Expanded ‘pre-notification for change approval’
- by Lee, Hye-Kyung Mar 25, 2024 05:59am
- The pilot system for ‘pre-notification for pharmaceutical change approval,’ which allows companies to predict the schedule of post-approval changes, will now applied to pharmaceuticals required for reporting production, imports, and supply disruptions. Since December 18th of last year, the Ministry of Food and Drug Safety (MFDS) has been implementing a pilot system for pre-notifying processing post-approval changes. The system was designed to consider the product’s manufacturing and import schedule and process the application within the due date specified by the applying company. Previously, post-approval changes were processed without notification once the MFDS completed the review according to the approval and review procedure. This made it difficult for applying companies to predict the date of change approval. The system has been updated to make the drug approval system flexible and reasonable. Starting this year, the MFDS pilot system for ‘pre-notification for pharmaceutical change approval’ will be expanded to drugs requiring reports of production, imports, and supply disruptions. The pre-notification system for post-approval changes, piloted until December 31st, includes the processing of change approvals for new drugs, orphan drugs, and cutting-edge biomedicines past the legal processing due date. Starting this year, the system will be expanded to include pharmaceuticals requiring reports of production, import, and supply disruptions, in order to ensure a stable domestic supply of pharmaceuticals. The list of pharmaceuticals subject to reporting production, import, and supply disruptions, posted annually by the Health Insurance Review and Assessment Service (HIRA), includes about 2,805 items (excluding duplicates) as of 2023, including anticancer drugs with 1-2 suppliers. Companies that wish to be pre-notified for pharmaceutical change approval can select ‘yes’ to the ‘modification of change date’ when filing an application to the MFDS. When adjustment dates were not specified at the time of application, companies can apply for the system via official letter until seven days before the processing deadline. If a company wishes to request a modification to the post-approval change date, it must specify the date after the legal processing date. For example, if the application's total processing period is 50 days, the company can specify the date within 50 working days of the processing deadline. However, companies cannot shorten the processing duration through this system because it was designed not to affect the existing approval review process. The pre-notification system only applies to cases where the application processing has to be delayed (extended) beyond the original processing deadline due to the drug's manufacturing or import schedule. Modifications to change approval date (extension) can generally be applied to products, except when they fall under one of the following criteria: ▲restrictions to efficacy, method-of-use, and dose that relate to the safety of the product ▲a change in warning labels ▲or when requiring importance and urgency. The MFDS will pilot the system until the end of December this year and decide on formal operation after an evaluation and review of the results. “For pharmaceutical, we receive many requests for simple changes or extension of the deadline for drugs with confirmed approval,” an official from the MFDS stated. “The pre-notification system is an additional administrative procedure designed to aid the industry. So we encourage companies to apply for the system when they need it.”
- Policy
- Samsung Bioepis’s Soliris biosimilar is introduced
- by Lee, Tak-Sun Mar 25, 2024 05:59am
- The cost of Soliris (eculizumab), a drug known for its high price, is expected to drop significantly with the introduction of its biosimilar. The original Soliris will also cut its price by 30% in line with the expansion of its reimbursement benefit to cover neuromyelitis optica, to compete with its biosimilars. According to industry sources on the 22nd, Samsung Bioepis' Soliris biosimilar ‘Episcli Inj’ will be reimbursed from April. The upper limit will be set at KRW 2,514,858 per vial. This is only 48.8% of the current upper limit set for Soliris, which is set at KRW 5,132,364. The 1-year drug cost of Episcli Inj is also KRW 271 million, half the cost of Soliris' KRW 554 million. As a result, the burden on patients is expected to be significantly reduced if the patients choose to use biosimilars. However, Soliris is also taking measures to gain a competitive edge. The drug’s reimbursement was extended to cover neuromyelitis optica spectrum disorder (NMOSD). Currently, it covers orthopedic hemolytic uremic syndrome (aHUS) and paroxysmal nocturnal hemoglobinuria (PNH). During negotiations with the National Health Insurance Service to expand the scope of coverage, Soliris’s company agreed to reduce the upper limit by 29.9%. Starting next month, the upper price limit of the drug will be reduced to KRW 3.6 million per vial. The cost of a year's supply will also be reduced from KRW 554 million to KRW 288 million. Patients will pay 10.5 million won per person per year when applying the copayment ceiling. Soliris' decision to lower the drug price was also influenced by the reimbursed entry of Enspryng (satralizumab), its competitor in optic neuromyelitis. Enspryng has been reimbursed as of December 1 of last year. Its out-of-pocket cost per patient per year is up to KRW 101.4 million when applying the copayment ceiling system. If Soliris’s price is reduced, its out-of-pocket cost will no longer be significantly different from Enspryng.
- Policy
- Economic benefits paid to doctors to be publicly disclosed
- by Lee, Jeong-Hwan Mar 22, 2024 06:08am
- On the 21st, the government announced the guidelines for the public disclosure of expenditure reports on the legitimate financial benefits paid by pharmaceutical and medical device companies to doctors and pharmacists that will be disclosed in December. The guidelines stipulate the detailed schedule, content, and method for disclosure of the economic benefit expenditure report prepared by companies as of the fiscal year 2023, per the amendments to the Pharmaceutical Affairs Act and the Medical Device Act, made on July 20, 2021. Under the current law, the legally permissible economic benefits that can be provided are the provision of physical products, support for conferences, support for clinical trials, product presentations, post-marketing surveys, cost discounts based on payment terms, and use for performance verification before purchase (medical devices only). When the expenditure report is disclosed, the public will be able to check the medical institution (name, symbol of the medical institution) that received economic benefits from drug and medical device suppliers, information on support for conferences, and the amount of support provided to participants at product presentations. However, under the Enforcement Rules of the Pharmaceutical Affairs Act and the Medical Device Act, the names of recipients such as medical practitioners whose personal information is at risk of exposure and clinical trial information containing confidential business strategies will be de-identified and disclosed in the expenditure report. This is in accordance with Article 44 (2) (3) of the Enforcement Rule of the Pharmaceutical Affairs Act, which stipulates, "If the Minister of Health and Welfare is notified that the details of the expenditure report contain information subject to non-disclosure under Article 9 of the Official Information Disclosure Act, it shall be disclosed after taking necessary measures to ensure that the contents cannot be identified. Kyung-sil Chung, Director Bureau of Healthcare Policy at the Ministry of Health and Welfare (MOHW), said, "The disclosure of the expenditure reports is to create an environment for the industry to self-censor rebates through the disclosure of legitimate economic benefits. We will be receiving related data through the Health Insurance Review and Assessment Service from June this year, and we ask for the companies’ cooperation to ensure accurate information disclosure." The operating guidelines for the expenditure report will be available on the websites of HIRA and other related associations.
- Policy
- Enhertu’s price falls to KRW 70 mil range with reimb
- by Lee, Tak-Sun Mar 22, 2024 06:06am
- The list price of the petitioned anti-cancer drug Enhertu was reportedly set at KRW 1.4 million per vial. This is significantly cheaper than the non-reimbursed price of KRW 2.3 million. In addition, the National Health Insurance Service (NHIS) will apply a risk-sharing agreement (RSA) system for the reimbursement of the drug, so the actual price of the drug is expected to be lower. According to industry sources on the 21st, Enhertu’s price is going to be set at an upper limit of about KRW 1.4 million per vial. The price had been reportedly applied to the drug when it passed HIRA’s Drug Reimbursement Evaluation Committee review in February. In other words, the NHIS seems to have been negotiating around the price set by DREC. This may explain why the negotiations began in late February and were completed in just a month. Considering that an average weight patient requires 3 vials per treatment cycle (21 days), the drug’s non-reimbursed price is about KRW 7 million, and the listed reimbursed price is KRW 4.2 million. In terms of annual treatment costs, the non-reimbursed price is about KRW 120 million and the list price is about KRW 71.4 million. The actual price is likely to be lower with the application of the RSA system. The expenditure cap type and refund type will be applied to Enhertu. Enhertu’s reimbursement listing will be officially notified after being reported to the Health Insurance Policy Deliberation Committee's meeting scheduled for next week. Enhertu is an antibody-drug conjugate (ADC) anticancer drug that is highly effective against HER2-positive breast cancer, which accounts for around half of all metastatic breast cancers. It is also used for HER2-positive gastric or gastroesophageal junction (GEJ) adenocarcinoma. In particular, the drug demonstrated a better effect over existing drugs in clinical trials. Compared to chemotherapy, Enhertu reduced the risk of disease progression or death by 50%. The overall survival (OS) was 23.4 months with Enhertu, 6.6 months longer than the 16.8 months of the control group. The superior effect prompted the call for fast-track registration of Enhertu in the medical field. The petition was signed by 50,000 people and reported to the National Assembly.
- Policy
- National Essential Medicines to be categorized into 4 groups
- by Lee, Hye-Kyung Mar 21, 2024 05:53am
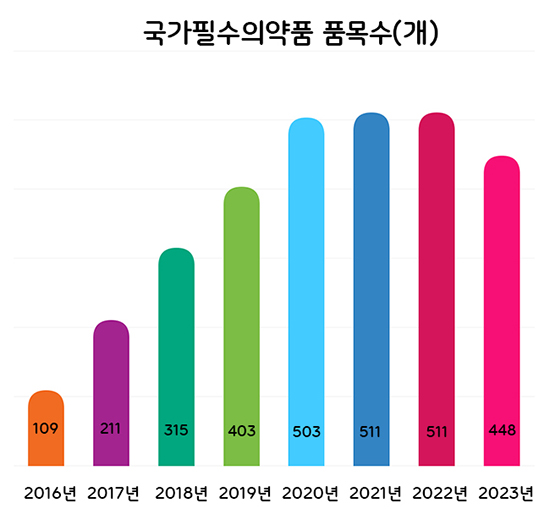
- The Ministry of Food and Drug Safety (MFDS) plans to categorize national essential drugs into 4 groups and conduct regular level assessments to better manage the drugs. According to the 'Research Service to Prepare a Measure to Classify and Manage the National Essential Medicine ‘ that was recently announced by MFDS, the authorities will discuss improvements and revisions to the classification criteria used to set the supply stability grade of national essential drugs by May. The four-level classification plan was made in response to the need to establish a differentiated management system for already designated national essential drugs, which was pointed out in the 2nd Comprehensive Plan for Stable Supply of National Essential Drugs in 2022. Through the project last year, the MFDS prepared four-level classification criteria for national essential drugs: ▲drugs that require prior stockpiling, ▲drugs that require immediate supply in case of a crisis, ▲ drugs that require constant monitoring of the supply situation and promotion of localization, and ▲drugs that require continuous attention. The classifications are based on the impact on public health, urgency of use, and potential availability of supply. Number of National Essential Medicines by Year Based on the research service results, the MFDS will finalize the classification and management methods of already designated national essential medicines and prepare feasibility studies and designations for ingredients and formulations that request new designations. For already designated national essential drugs, the MFDS plans to apply the 4-level classification system and conduct regular level management. For this, the research will identify and revise improvements to the classification system. The proposed list of ingredients and formulations that are applied to the standards and improvements prepared through the research will be reviewed by the National Essential Medicine Subcommittee. Ingredients and formulations requesting new designations this year will be reviewed for healthcare necessity and supply stability based on the evaluation criteria that had been determined through the Council for the Safe Supply of National Essential Medicines that was in November last year. The MFDS explained, "We need to continue to designate drugs that are essential for healthcare but are difficult to be supplied stably through market functions alone as national essential medicines and update the list of already designated national essential drugs. The final ingredients and formulations will be designated after resolution by the Council for the Safe Supply of National Essential Medicines Meanwhile, the number of national essential medicines has steadily increased from 109 in 2016 to 511 in 2022, and a total of 448 ingredients and formulations have been designated through new and de-designations last year.
- Policy
- Gov’t raises price of Harmonilan due to unstable supply
- by Lee, Tak-Sun Mar 21, 2024 05:52am
- Enteral nutrition products Harmonilan(left) and Encover(right) The insurance ceiling price of the enteral nutrition formula Harmonilan (B Braun Korea), which the company has been experiencing difficulties in ensuring supply and demand recently, is expected to rise from April. The company had continuously been applying to register the drug as a ‘drug shortage prevention drug' and preserve production costs due to its low profitability, to no avail. This is why criticism arose on how the government has deferred taking measures until now and only set out to adjust the price ceiling after the supply and demand instability intensified. Harmonilan’s actual transaction price had been cut 2 years ago According to industry sources on the 20th, the company has completed negotiations to raise the ceiling price of Harmonilan with the government, and the new drug price is expected to be applied next month after being reported to the Health Insurance Policy Deliberation Committee. Encover and Harmonilan are the two products that dominate the enteral nutrition market. Enteral nutrition products are given to patients who have difficulty getting nourished through food. The product is directly into the digestive tract through a tube. They are essential for patients with eating disorders. However, enteral nutrients such as Harmonilan and Encover are often in short supply depending on import situations, which has caused a lot of frustration among patients. This is why healthcare providers and patients have long requested such enteral nutrition products be designated as a drug shortage prevention drug, but health authorities have been unwilling to do so. Pharmaceutical companies have also requested the designation. Because they are low-margin products, the companies explained that they would need to raise the price of the drugs to conserve their cost and keep up with the high demand. However, the price of these enteral nutrition products has fallen in the past due to actual transaction price cuts and the Price-Volume Agreement system. The price of Harmonilan 200ml was lowered from KRW 2,291 to KRW 2,282 in January 2022 as part of actual transaction price cuts. In the case of Encover, the price of the 200ml product had fallen 2.9% in October 2022 under the PVA system. The company had applied for price adjustments at the time, but the price had not been increased then. Such price reductions are regarded as a major cause of supply instability, as they decrease profitability. Therefore, the price increase granted for Harmonilan this time is regarded as one example of the government's inconsistent drug price adjustment policy. Drug that require price increases are also subject to price cuts The government has been postponing the implementation of the actual transaction price cut plan, which had been scheduled to take effect in January. This in part is interpreted as the government’s effort to to prevent cases like Harmonilan, as drugs with unstable supply and demand may be subject to price reductions. According to government officials, it is likely that the price reduction will not be implemented in April either. The postponement has also halved the health insurance financial savings the government sought to earn through the drug price reduction. The government seems to be in a dilemma, caught between its recent move to broadly raise drug prices of drugs with unstable supply and measures previously prepared to cut the prices of existing drugs. The industry is calling for a complementary measure to prevent price cuts not only for existing drug shortage prevention drugs but also for drugs that are likely to have unstable supply and have difficulty continuously treating patients. An industry official said, "The list of non-eligible items should be expanded after close examination when selecting subjects for actual transaction price cuts and PVA price cuts reductions. We need to get rid of the absurd situation where a drug subject to a price reduction suddenly becomes a drug subject to a price increase.”
- Policy
- MSD withdraws SGLT2 inhibitors in a row
- by Lee, Hye-Kyung Mar 20, 2024 05:44am
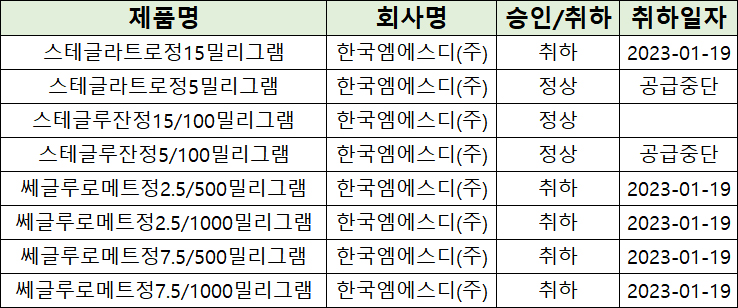
- MSD Korea is facing tough competition in the market for SGLT-2 inhibitors in South Korea. MSD decided that they will discontinue the supply of Steglatro Tab 5 mg and 'Stegluzan Tab 5/100 mg (ertugliflozin plus sitagliptin)' after voluntarily withdrawing 'Steglatro Tab 15 mg (ertugliflozin)' and metformin combination therapy, 'Segluromet,' last year. The list of approved and withdrawn SGLT-2 inhibitors by MSD in South Korea. Except for Stegluzan Tab 15/100 mg, all of MSD According to the Ministry of Food and Drug Safety (MFDS) report on the 15th, supply discontinuation was reported for Steglatro Tab 5 mg and Stegluzan Tab 5/100 mg. Imports of Steglatro Tab 5 mg will end on May 31st and Stegluzan Tab 5/100 mg will end on August 30th, after which these drugs will be discontinued. MSD says, “Due to a reduction in market demand, we will discontinue these drugs after the final import.” And MSD also stated, “The last import date is flexible depending on the manufacturing schedule and planned between mid-May and mid-August.” MSD stated that substitution is possible since other SGLT-class products are already available in the market. They also mentioned that they will notify healthcare professionals before discontinuing sales to ensure appropriate measures can be taken. If MSD voluntarily withdraws two items that they have decided to discontinue importing, Stegluzan Tab 15/100 mg will be their only SGLT-2 inhibitor containing ertugliflozin. However, Stegluzan Tab 15/100 mg has no distribution record after approval, and the company does not intend to distribute. The market for SGLT-2 inhibitors has grown to KRW 170 billion. According to the pharmaceutical market research agency UBIST, Steglatro generated merely KRW 1.6 billion in outpatient prescriptions. Industry analysis suggests that Steglatro lacks a competitive edge compared to Forxiga and Jardiance because its indication is limited to type 2 diabetes and clinical trials are lacking in expanding treatment areas. Changes in prescription performance by SGLT-2 inhibitors. SGLT-2 inhibitors have emerged as treatments for type 2 diabetes and are broadening their use in various diseases targeting the heart and kidney. SGLT-2 inhibitors inhibit the reabsorption of glucose in the kidneys, leading to glucose excretion in the urine. This results in reduced blood sugar, weight loss, kidney function protection, and blood pressure reduction. As of 2022, the items have recorded over KRW 40 billion in outpatient prescriptions individually, including AstraZeneca’s monotherapy 'Forxiga (ingredient: dapagliflozin),' a combination therapy ‘Xigduo,’ and Boehringer Ingelheim's monotherapy Jardiance (ingredient: empagliflozin). AstraZeneca’s drug generated KRW 91.4 billion, approximately KRW 15 billion more than Boehringer Ingelheim’s KRW 76.1 billion.